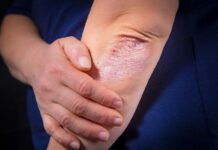
The liver is an amazing organ
The roles of the liver in the human body includes detoxification, protein synthesis, and synthesizing enzymes for the digestion of food. It is the largest solid organ and the largest gland in the human body. It is located in the upper right-hand portion of the abdominal cavity, beneath the diaphragm, and on top of the stomach, right kidney, and intestines. It has two main lobes that are made up of tiny lobules and it has two different sources of blood supply. The hepatic artery supplies oxygen-rich blood that is pumped from the heart, while the portal vein supplies nutrients from the intestine and the spleen. The portal vein allows nutrients and chemicals from the digestive tract to enter the liver for processing and filtering prior to entering the general circulation of the whole body.
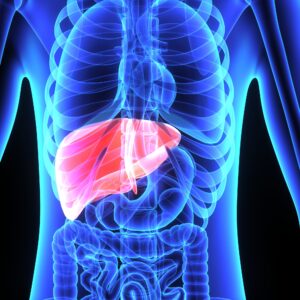
Why liver health is important
Because of the many roles of the liver, it is essential in keeping the body running in great condition. The critical functions of the liver include:
- Production of bile
- Production of certain proteins for blood plasma like albumin
- Production of cholesterol and special proteins
- Production of glycogen
- Regulating the amino acid level
- Processing of hemoglobin
- Production of urea from ammonia
- Detoxification of the blood by clearing the drugs and other poisonous substances
- Regulation of blood clotting
- Storage of vitamin and minerals
- Clearance of bilirubin
Because of the importance of the liver and its functions, it can regrow rapidly as long as it is kept healthy. The liver can regenerate completely, as long as the minimum of 25% of the tissue remains. One of the impressive aspects of this feat is that the liver can regrow to its previous size and ability without any loss of function during the growth process. However, when the repair fails, the liver experiences a range of problems. In a diseased or malfunctioning liver, the consequences can be dangerous or fatal.
What happens if your liver is affected by disease?
There are many types of liver diseases and the damage usually progress in a similar way. Liver disease, or hepatic disease, is any disturbance of liver function. As the liver is responsible for many critical functions within the body, any injury or loss of functions can cause significant damage to the body. A decrease in liver function usually occurs when more than 75% or three quarters of liver tissue is affected, and this compromises liver health.
Example of liver disease include:
- Hepatitis
- Alcoholic Liver Disease
- Fatty Liver Disease
- Cirrhosis
- Gilbert’s Syndrome
- Primary Sclerosis Cholangitis
- Liver Cancer
According to recent statistics, liver disease is on the rise. 1 in 4 Canadians may be affected by liver disease, ranging from different ages from newborns to older adults. There are over 100 liver diseases and they are caused by a variety of factors including viruses, toxins, genetics, alcohol, and other unknown causes.
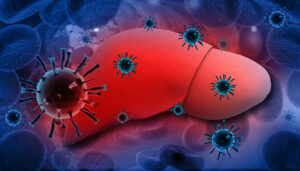
The signs and symptoms associated with liver disease vary and are dependent upon the exact type of liver disease that is present. The most common symptoms are:
- Jaundice
- Abdominal pain and swelling
- Itchy skin
- Dark urine colour
- Nausea
- Vomiting
- Chronic fatigue
- Pale stool colour
- Bloody stool
- Tar-coloured stool
- Swelling in the ankles and legs
- Loss of appetite
- Easy bruising
What is medical cannabis?
Medical cannabis is increasingly being prescribed in clinics for various clinical reasons apart from cancer and chemotherapy symptom relief. Healthcare practitioners may authorize the use of cannabis in various forms for the relief of symptoms associated with a variety of disorders which have not responded to conventional medical treatments.
Cannabis is a generic term for the psychoactive substances prepared from the plant genus Cannabis sativa. The main and most potent psychoactive ingredient in cannabis is tetrahydrocannabinol (THC). Cannabidiol (CBD) is an additional cannabinoid that is also present in preparations of Cannabis sativa. It is non-psychoactive but it has only about 10% of the activity of THC.
Recent studies have suggested that CBD has anti-anxiety and anti-psychotic effects. It has also been shown to have anti-inflammatory effects and it can modulate the immune system response. Furthermore, it has an excellent safety profile in humans even after chronic use. CBD has been investigated as possible therapeutic targets in various GI diseases such as irritable bowel syndrome, inflammatory bowel disease, and other diseases involving the GI tract. They have also been investigated in the management of other symptoms such as nausea and vomiting, cannabinoid hyperemesis syndrome, anorexia, weight loss, and chronic abdominal pain. As some of these indications are commonly seen in patients with cancer, those receiving chemotherapy, and patients with HIV infection, cannabis has found widespread acceptance in the management of these patients.

How does medical cannabis work to improve liver health?
Currently, there is limited information regarding the use of cannabis in liver disease. There are many unanswered questions with regards to the health outcomes of cannabis long-term users and the effect of medical cannabis on liver health.
Endocannabinoids have been associated with pain, inflammation, mood enhancement, and the utilization and conservation of energy. Endocannabinoids are associated with the accumulation of fat by increasing lipogenesis throughout the body, decreasing the rate of lipolysis, and stimulating appetite. Cannabinoids are thought to act on the CB1 and CB2 receptors. CB1 is mainly expressed in the brain and also in the periphery, while CB2 has been detected in the periphery, immune cells, liver, pancreas, brain, hematopoietic system, and bone. CB1 and CB2 receptors have been implicated in various pathological processes, making them interesting therapeutic targets.
Whereas the functions of CB1 receptor have been extensively studied, the CB2 receptors has emerged to play a role in the regulation of inflammation, pain, atherosclerosis, and osteoporosis. The development of selective CB2 molecules has gained interest as new targets in drug discovery, and CB2 receptors were found to have a major role during chronic and acute liver injury, including fibrogenesis associated to chronic liver diseases, liver reperfusion injury, and hepatic encephalopathy associated to acute liver failure.
CBD has shown anti-inflammatory, antioxidant, and hepatoprotective effects in clinical studies. Both CBD and THC have shown evidence of therapeutic potential in chronic liver diseases involving inflammatory changes and fatty degeneration, hence the potential to improve liver health.
Studies about medical cannabis and the liver
The Lancet published one of the earliest studies in 1971 which investigated the effects of cannabis on the liver. They found abnormal liver enzymes and hepatic dysfunction in young chronic cannabis users and this was amplified by ingestion of alcohol. More studies have been performed since then.
A 2004 study showed that cannabis consumption was associated with hepatomegaly (enlargement of the liver) and splenomegaly (enlargement of the spleen) in 57.7% and 73.1% of the patients, respectively. Similar to the previous study, they also showed slight elevations in some of the liver enzymes, namely alanine transaminase, aspartate transaminase, and alkaline phosphatase. However, they also showed that there might be confounding factors in their results, such as underlying viral infections, which are common among cannabis users.
However, the question of whether regular use of cannabis has any detrimental effects specifically on the liver, especially in the presence of pre-existing disease, still remains controversial. Some studies found worsening of comorbidities while on the contrary, some found that cannabis use did not cause worsening of hepatic pathology in the presence of comorbidities.
The effects of medical cannabis on liver health still warrants further studies.
How does medical cannabis help with alcoholic liver disease?
The chronic consumption of alcohol is a major cause of alcoholic liver disease, which eventually may progress to cirrhosis or hepatocellular carcinoma in susceptible subjects. It is characterized by metabolic dysregulation, enhanced oxidative stress, inflammation and steatosis in the liver. A significant number of people who abuse alcohol also have a combined usage of tobacco and/or cannabis. Despite significant advances in our understanding of the pathology of alcoholic liver disease, the therapeutic options are still very limited.
Recent studies showed that the use of cannabinoids with alcoholic liver disease may have a possible protective effect. In a mouse model, cannabinoids reduced inflammation, oxidative stress, and steatosis in ALD. In this cohort study, cannabis use was associated with decreased rates of alcoholic steatosis, hepatitis, cirrhosis and hepatocellular carcinoma.
Another study in 2014 by Yang et al showed that CBD has a positive effect on alcohol-induced hepatic steatosis, or fatty liver disease. Fatty liver disease is when there is too much fat build-up in liver cells and it can be caused by heavy drinking alcohol. Although the fat deposits usually disappear if alcohol consumption is stopped, it can lead to enlarged liver, hepatitis, and ultimately cirrhosis if alcohol usage continues.
CBD was found to have a preventative effect in alcohol-induced liver injury and it also causes the lowering of the blood alcohol levels when taken with alcohol. The main mechanism of action of CBD is by preventing the increase in oxidative stress and increases the autophagy induced by alcohol which leads to healthier liver cells.
How does medical cannabis help with non-alcoholic liver disease?
Sometimes, the development of fats in the liver cells does not involve alcohol at all. Non-alcoholic fatty liver disease is the most common liver disease in Canada, affecting over 7 million people, and these are people who drink little to no alcohol. In the United States, it is the most common form of chronic liver disease, affecting about one-quarter of the population. The cause is unknown but it has associated with obesity, insulin resistance, hyperglycemia and high level of triglycerides or fats.
In one study, Adejumo et al showed that cannabis use was associated with a decreased prevalence of non-alcoholic fatty liver disease. They found a 43% decrease in dependent users compared with nondependent users. The more patients used medical cannabis, the less likely they were to have non-alcoholic liver disease. In a separate study, they also demonstrated significantly lower odds of developing steatosis, steatohepatitis, cirrhosis, and hepatocellular carcinoma in alcohol abusers who also used marijuana.
How does medical cannabis help with viral liver disease?
Currently, there is no human data regarding the role of cannabis with chronic hepatitis B, but it has been found that in vitro cannabis has no effect on the virus. Most of the studies have been done in patients with chronic Hepatitis C (HCV) and HIV. Moreover, the different effects of cannabis between the infected groups is unclear and further studies will need to be performed.
With regards to patients with viral liver diseases taking medical cannabis to relieve some of their symptoms, it was found that it does not accelerate the progression of liver disease in patients with coinfection of HIV and Hepatitis C. Earlier studies suggested that cannabis use resulted in increased steatosis, fibrosis and worsening of HCV disease. However, recent observations and reports revealed that cannabis use has no effect on HCV disease progression. Some reports even revealed that cannabis use was associated with reduced steatosis in HCV-infected individuals. However, it is important to note that the results also showed the possibility of increased cannabis use to be associated with higher risks of fibrosis progression in the liver. The general consensus is that only large daily consumption of cannabis is usually associated with development of liver fibrosis and can affect liver health.
Historically, cannabis was also used as an adjunct agent in hepatitis C treated with interferon and ribavirin. It was linked with higher rates of treatment completion and cure. It improved the adherence of patients to the antiviral treatments. Ultimately, medical cannabis can promote liver health by making it easier for patients to go through antiviral treatments.
What about medical cannabis and the liver health of transplant patients?
The use of medical cannabis by liver-transplant patients remains controversial, with only a minority of North American programs transplanting patients who use cannabis. The main concerns are the possible impact of cannabis usage on graft survival, the compliance of medications, and the likelihood of addiction. However, cannabis use does not seem to have an adverse impact on liver transplant waitlist survival in two retrospective case series from Michigan and San Francisco.
Although cannabis use is not an absolute contraindication to transplantation, it should be used with caution and on a case by case basis. The risks and benefits need to be assessed in the context of medical use and it should be thoroughly explored for liver-transplant patients.
The future of medical cannabis and liver health
There are favourable studies describing the effects of medical cannabis on liver health. However, the impact of medical cannabis on liver disease remains unclear and controversial. Additionally, it seems to have variable effects depending on the underlying disease as described by the studies above. Cannabinoids may have a future role in the management of NAFLD and ALD due to its anti-inflammatory and antioxidant effects, but more studies are warranted. Given the current evidence, it is not recommended for use in patients with hepatitis C even though it has shown to have no effect in the progression of the liver disease. Moreover, cannabis is not an absolute contradiction in the assessment of patients awaiting liver transplant but they should be assessed in a case by case basis.
It is always recommended to consult your healthcare provider before taking medical cannabis for the purposes of promoting liver health, especially if any underlying liver diseases are present.
Sources:
Adejumo, A. C., Ajayi, T. O., Adegbala, O. M., Adejumo, K. L., Alliu, S., Akinjero, A. M., … Bukong, T. N. (2018). Cannabis use is associated with reduced prevalence of progressive stages of alcoholic liver disease. Liver International, 38(8), 1475–1486. doi:10.1111/liv.13696
Wang, Y., Mukhopadhyay, P., Cao, Z. et al. Cannabidiol attenuates alcohol-induced liver steatosis, metabolic dysregulation, inflammation and neutrophil-mediated injury. Sci Rep 7, 12064 (2017). https://doi.org/10.1038/s41598-017-10924-8
Cohen, K., Weizman, A., & Weinstein, A. (2019). Positive and Negative Effects of Cannabis and Cannabinoids on Health. Clinical Pharmacology & Therapeutics. doi:10.1002/cpt.1381
Zhu, J., & Peltekian, K. M. (2019). Cannabis and the liver: Things you wanted to know but were afraid to ask. Canadian Liver Journal, 1–7. doi:10.3138/canlivj.2018-0023
Christopher N Andrews, MD, MSc, Shane M Devlin, MD, Bernard Le Foll, MD, PhD, Benedikt Fischer, PhD, Frances Tse, MD, MPH, Martin Storr, MD, Stephen E Congly, MD, MSc, Canadian Association of Gastroenterology Position Statement: Use of Cannabis in Gastroenterological and Hepatic Disorders, Journal of the Canadian Association of Gastroenterology, Volume 2, Issue 1, April 2019, Pages 37–43, https://doi.org/10.1093/jcag/gwy064
Goyal, Hemant & Rahman, M Rubayat & Perisetti, Abhilash & Shah, Nihar & Chhabra, Rajiv. (2018). Cannabis in liver disorders: a friend or a foe?. European Journal of Gastroenterology & Hepatology. 1. 10.1097/MEG.0000000000001256.
Yang, Lili et al. “Cannabidiol protects liver from binge alcohol-induced steatosis by mechanisms including inhibition of oxidative stress and increase in autophagy.” Free radical biology & medicine vol. 68 (2014): 260-7. doi:10.1016/j.freeradbiomed.2013.12.026